A small cavity can feel like a non-issue. It’s not hurting. It’s tiny. You’ll deal with it at your next cleaning. And then the next cleaning comes and goes, and somehow the cavity is still on the list. Most people have been in this cycle at some point, and the problem isn’t laziness. It’s that small cavities don’t always announce themselves until they’ve already grown into something much harder to treat.
This blog takes an honest look at what really happens inside a tooth when a cavity is left untreated. The progression is predictable, the consequences are real, and the good news is that catching decay early is almost always the easier, less involved route.
Why Small Cavities Don’t Stay Small
Tooth decay is a bacterial process. The bacteria in your mouth feed on sugars and produce acids that gradually eat through enamel, the hard outer layer of your tooth. Early-stage decay, sometimes called a white spot lesion, can sometimes be reversed with fluoride and better oral hygiene if detected early. But once a cavity has broken through enamel and moved into dentin, the softer tissue beneath it, that reversal window closes.
At Irvine Smiles Dental, where family dentistry in Irvine means treating patients across every age and stage, we see this pattern regularly. A cavity diagnosed at one appointment that was manageable with a simple filling returns two years later as something far more involved, simply because treatment was postponed.
The Stages of a Cavity Left Untreated
Understanding how decay progresses helps clarify why timing matters so much. A cavity doesn’t stay confined to enamel. It moves deeper, stage by stage, until the damage is either addressed or the tooth is lost.
Enamel Decay
This is the earliest stage. Enamel is the hardest substance in your body, but it has no nerve endings, which is why you typically feel nothing at this point. A filling here is straightforward: the decayed material is removed, and the tooth is restored. This is the stage most people are in when their dentist first mentions a cavity.
Dentin Decay
Dentin is porous and much softer than enamel. Once decay reaches it, progression accelerates. Dentin contains microscopic tubules that connect to the tooth’s nerve, so this is usually when sensitivity to hot, cold, or sweet foods begins. Treatment at this stage still typically involves a filling, but the preparation is larger and the procedure more involved.
Pulp Involvement
The dental pulp sits at the center of the tooth and contains blood vessels, connective tissue, and nerves. When decay reaches the pulp, infection sets in. This is where the dull ache becomes a persistent throb, where pain without an obvious trigger starts, and where a root canal becomes necessary. Root canal therapy removes the infected pulp, cleans the canals, and seals the tooth. It saves the tooth, but it’s a significantly more involved procedure than a filling.
Abscess Formation
If an infection in the dental pulp is left untreated, it can extend beyond the root and affect the surrounding bone and gum tissue, leading to the formation of a dental abscess. This abscess is a pus-filled pocket caused by bacterial infection and is often associated with intense, spreading pain, noticeable swelling, and sometimes fever. The American Dental Association warns that such abscesses can escalate into serious medical emergencies if the infection continues to spread. At this point, treatment typically involves draining the abscess, prescribing antibiotics, and, in many cases, extracting the affected tooth if it cannot be saved.
Source: Teeth Talk Girl
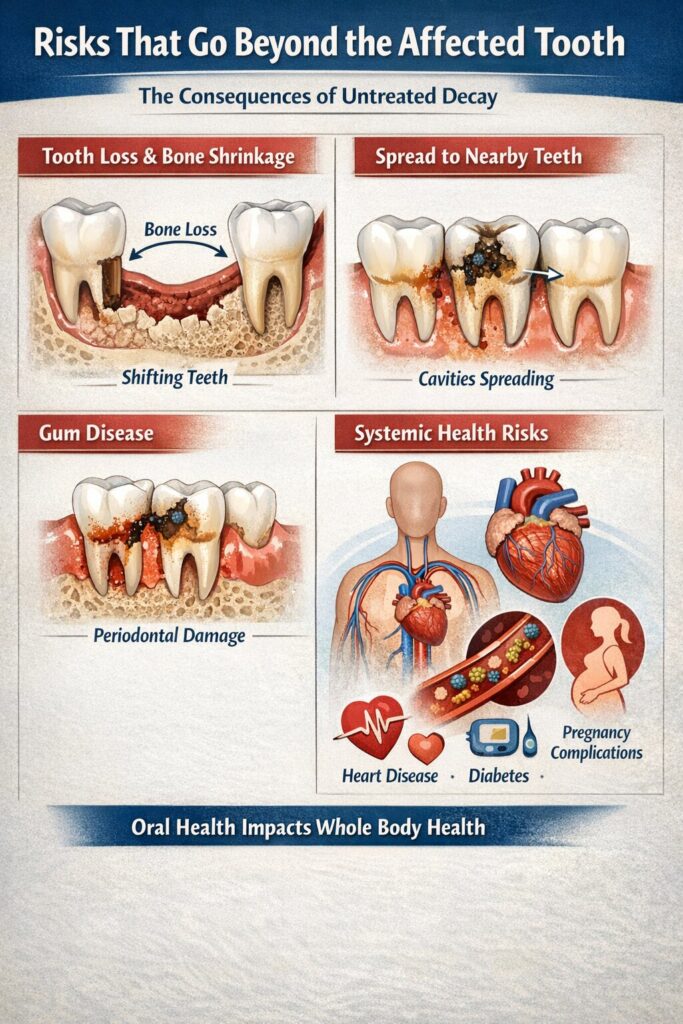
Risks That Go Beyond the Affected Tooth
The consequences of untreated decay rarely stay contained. Several secondary problems tend to develop as the original cavity progresses, and each one adds complexity to your overall treatment.
- Tooth loss: Once decay reaches an advanced stage or the structural integrity of the tooth is severely compromised, extraction may be the only option. Losing a tooth triggers its own chain of problems, including shifting of adjacent teeth and jawbone resorption in the area.
- Damage to neighboring teeth: Bacteria don’t respect tooth boundaries. Active decay in one tooth can spread to adjacent teeth, particularly where teeth are in contact. One untreated cavity can lead to two or three affected teeth within a few years.
- Gum disease: The inflammation and bacteria associated with untreated cavities can contribute to periodontal disease, which affects the gum and bone structure supporting the tooth.
- Systemic health implications: Research has linked poor oral health to increased risk of cardiovascular disease, diabetes complications, and adverse pregnancy outcomes. The bacteria from dental infections can enter the bloodstream, creating effects well beyond the mouth.
There’s no judgment in dentistry for how long it’s been. Patients come in after months or years away, and the first conversation is always about where things stand now, not a lecture about how they got there. What matters is getting a current picture of your oral health so you know what you’re dealing with.
A comprehensive exam at Irvine Smiles Dental will identify any active decay, assess the condition of existing restorations, and give you a clear treatment plan with options. If there’s a small cavity that can still be treated with a simple filling, the sooner it’s addressed, the simpler and more affordable the whole process will be.
Contact Irvine Smiles Dental today to schedule your exam. Our team sees patients of all ages, takes the time to explain what’s happening in your mouth, and treats every visit as a chance to help you stay ahead of problems rather than catch up to them.
People Also Ask
Early-stage enamel demineralization, before a physical hole has formed, can sometimes be reversed through remineralization with fluoride and improved brushing habits. However, once a true cavity has developed, meaning the bacterial decay has broken through the enamel surface, it cannot reverse itself. The cavity will continue to grow without treatment.
Most early cavities produce no symptoms at all. That’s what makes them easy to ignore and why regular dental exams are essential. Your dentist uses visual inspection, probing, and digital X-rays to identify decay that isn’t visible or painful yet. Waiting for a cavity to hurt before seeking treatment means waiting until it’s already progressed beyond the simplest stage.
A filling repairs a relatively small area of decay by removing the damaged material and restoring the space with composite resin or another material. A dental crown is a cap that covers the entire visible portion of the tooth, used when decay or damage is extensive enough that a filling can’t adequately restore the tooth’s structure or function. Cavities caught early typically need fillings. Larger or more progressed decay often requires a crown.
Yes, significantly. Frequent consumption of sugary or acidic foods and beverages feeds the bacteria that produce decay-causing acids. Sipping on sodas, sports drinks, or juice throughout the day keeps acid levels elevated in the mouth and accelerates enamel erosion. Reducing sugar frequency, staying hydrated with water, and rinsing after meals all slow the progression of existing decay.
Cavities can form as soon as primary teeth erupt, and tooth decay is one of the most common chronic conditions in children in the United States according to the CDC. Early childhood caries, sometimes called baby bottle tooth decay, can develop in toddlers. Regular dental visits starting around a child’s first birthday allow early detection and help parents establish effective brushing and diet habits before problems develop.
